Pain with Dupuytren disease receives little attention. This is a hot button topic. Many Dupuytren patients feel marginalized when they hear a doctor say that Dupuytren disease doesn’t hurt – because theirs does. Dupuytren disease can be very painful – but the majority of Dupuytren patients have no pain, and the reason for this is unknown. A smaller proportion of Dupuytren patients report pain than patients with other common painful hand conditions such as arthritis. Also, Dupuytren disease can coexist with other common painful hand conditions, and so pain with Dupuytren disease isn’t always pain from Dupuytren disease.
But the fact is that pain and itching are both common with Dupuytren disease. These charts show data is from chart review of over 3000 of my own Dupuytren contracture patients.
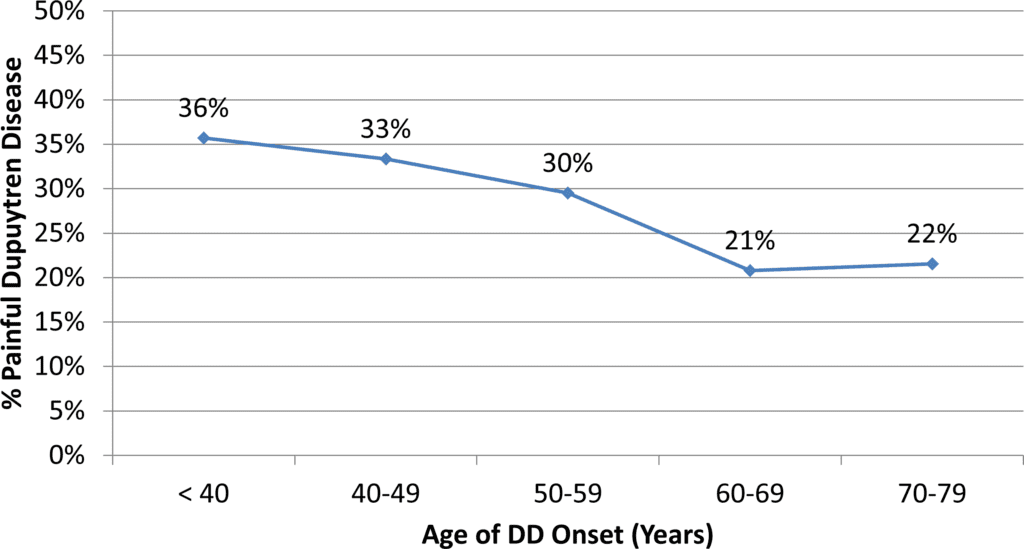
This chart shows the percent of patients who answered “yes” when asked if their Dupuytren disease was painful, broken down by age when Dupuytren disease first appeared.
This chart shows the percent of patients who answered “yes” when asked if their Dupuytren disease was itchy, broken down by age when Dupuytren disease first appeared..
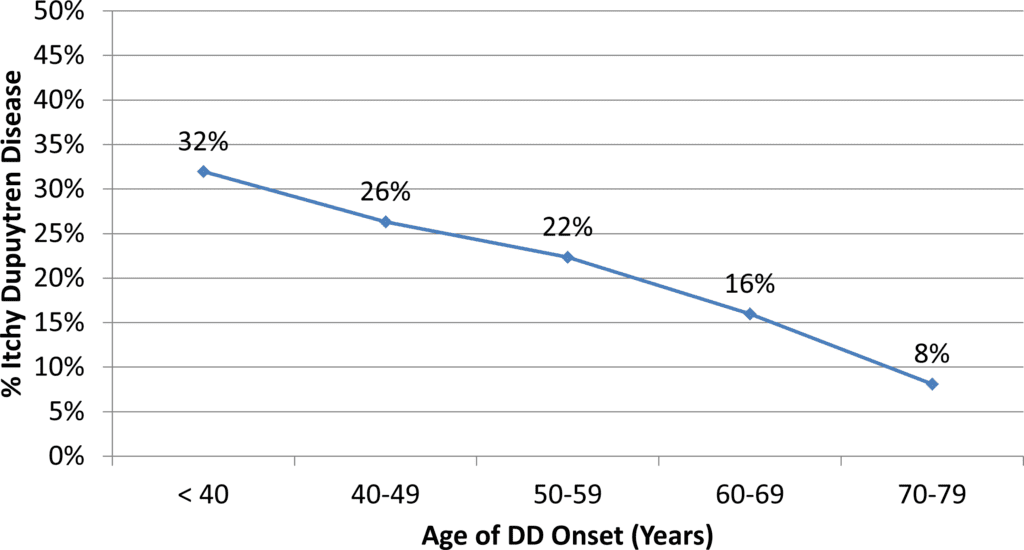
Overall, 21% (one out of five) reported itching in their Dupuytren affected areas, and overall, 28% (one out of three) reported pain in their Dupuytren affected areas. Itching and pain also correlated with earlier age of onset, which correlates with more aggressive disease biology. Take home bullets:
- Pain and itching are reported by a significant minority of Dupuytren patients.
- Pain is less common with Dupuytren disease than with hand arthritis or tendinitis.
- Pain and itching are more common in people with earlier age of Dupuytren diagnosis, which may mean that pain and itching are flags for aggressive disease.
- The majority of Dupuytren patients report neither pain nor itching.
What’s the explanation? One hypothesis is that pain and itching are due to immune-related pathways, consistent with a growing body of information that specific immune abnormalities and fibrocytes play a role in some Dupuytren patients.
Fibrocytes are circulating white blood cells produced by bone marrow which have features of both immune cells in the bloodstream and fibroblasts in the tissues. In several fibrotic diseases – including Dupuytren disease – blood tests show abnormally high numbers of circulating fibrocytes.
The biology goes like this: a body area which is damaged (or thinks it’s being damaged) releases distress proteins into the circulation – like a distress beacon. These distress proteins circulate and eventually circulate through through the bone marrow. This triggers the bone marrow to release fibrocytes into the circulation. Fibrocytes pour into the circulation, and guided by the cell’s version of smell, sniff out and go to the area releasing the distress proteins. When travelling through a tiny capillary blood vessel that smells like trouble, they grab onto the side of the blood vessel, escape between cells in the blood vessel wall and crawl out into the tissues. There, they transform into myofibroblasts, which are the cells that make collagen, pull on tissues, and generally cause Dupuytren contracture.
This scenario changes the direction research needs to pursue. Using military metaphors, it may be that myofibroblasts are just the foot soldiers, nodules the local battles, cords the scarred battlefield after the battle. To find a cure, we don’t need to kill all the soldiers and leave a trail of burned out battlefields. We just need to stop the responsible commander in chief, who is not necessarily even in the hand. We need to broaden the search beyond the hand (the war zone) to the bloodstream (the communication network), which is why the Dupuytren Foundation IDDB research project will be analyzing circulating immune biomarkers. These will help identify different Dupuytren subsets to define expectations, guide individualized treatment recommendations, develop ways to stop the process at its source, and eventually explain why pain is a real problem for some Dupuytren patients.